Healthcare teams lose revenue every day, but not from one catastrophic failure. Rather, it’s from missed follow-ups, stalled referrals, and patient outreach scattered across disconnected systems. A healthcare CRM brings those workflows together, giving revenue, operations, and patient access teams one place to manage relationships, track pipelines, and automate outreach.
This guide covers 15 healthcare CRM platforms clinical teams actually use, how they differ from EHRs, and what to prioritize when comparing fit, cost, compliance, and rollout effort. You’ll learn which features matter most — referral tracking, HIPAA support, EHR integration, and AI that does real work — so you can build a shortlist with confidence.
What is a healthcare CRM and how it differs from an EHR?
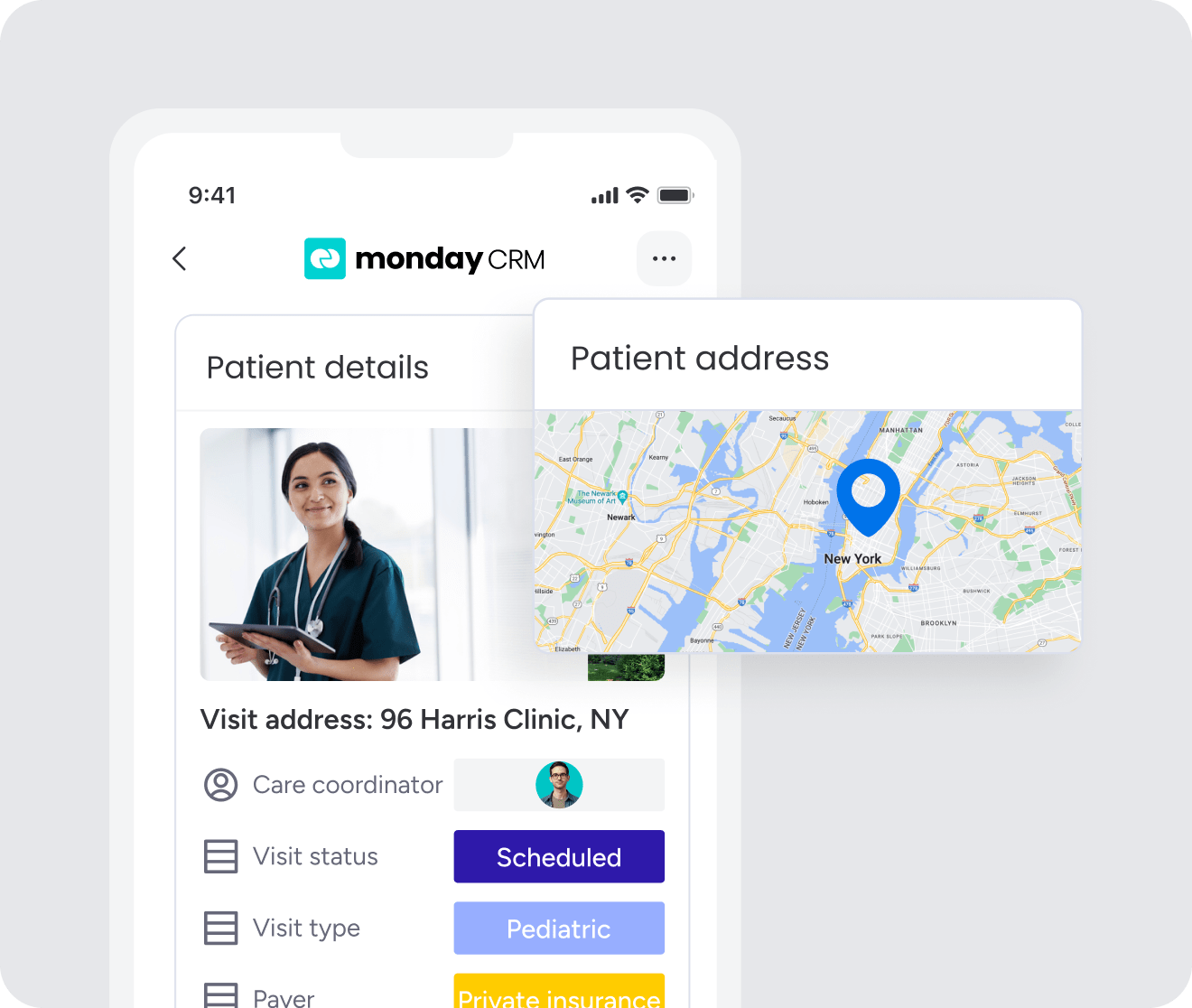
A healthcare CRM is a platform built to manage the operational and relationship side of a medical practice. It handles scheduling, referral tracking, patient outreach, and communication so clinical teams can stay focused on care delivery.
A healthcare CRM manages patient relationships and revenue operations, and an EHR manages everything that happens during the appointment, also known as clinical care. They serve different teams, track different data, and solve different problems.
| Dimension | EHR | Healthcare CRM |
|---|---|---|
| Who uses it | Physicians, nurses, clinical staff | Revenue teams, patient coordinators, marketing |
| What it tracks | Clinical records, diagnoses, medications | Contact info, interactions, referral sources |
| What it's for | Document and support care delivery | Manage patient relationships and revenue operations |
| The red tape | HIPAA clinical documentation rules | HIPAA contact data protection, marketing consent |
| How they play together | The system of record for clinical data | Connects to the EHR for a full patient view |
Pair a CRM with an EHR, and you get the full patient journey — clinical data stays accurate, and everyone can actually find what they need.
Try monday CRM15 best healthcare CRM platforms for providers and practices
Choosing a healthcare CRM gets messy fast. A solo practice and a regional hospital network need completely different things, and vendors know it. We’ve gathered the 15 best CRMs for healthcare companies, starting with this quick look chart, offering use cases, trial availability, standout features, and starting price so you can build your shortlist quickly.
| Platform | Use case | Free trial* | Notable feature | Starting price* |
|---|---|---|---|---|
| monday CRM | Flexible CRM for referral management and patient outreach | Yes | HIPAA-ready AI support on Enterprise plans | $12/seat/month |
| Salesforce Health Cloud | Enterprise unified engagement layer alongside EHR | Contact sales | FHIR-aligned interoperability with major EHRs | $350/user/month |
| HubSpot | Patient acquisition and marketing automation | Yes (free plan) | Email marketing automation and landing pages | $20/month |
| Zendesk | Omnichannel patient support and contact centers | Yes | Unified inbox across phone, email, chat, messaging | $49/agent/month |
| Microsoft Cloud for Healthcare | CRM and care coordination in Microsoft ecosystem | Contact sales | FHIR-based data virtualization with FHIRlink | $50/user/month |
| Epic (Cheers) | Patient engagement inside Epic EHR ecosystem | Contact sales | Capacity-aware outreach tied to scheduling | Custom quote |
| Zoho for healthcare | Adaptable CRM for smaller practices | Yes | Omnichannel communication with WhatsApp, SMS | $14/user/month |
| LeadSquared | Patient acquisition and intake automation | Yes | Multichannel HIPAA-compliant outreach | $60/user/month |
| Creatio | No-code CRM for complex process automation | Yes | Visual workflow builder with agentic AI | $25/user/month |
| NexHealth | Patient engagement for dental and medical practices | Contact sales | Real-time online scheduling synced to EHR | Custom quote |
| Tebra | All-in-one EHR, billing, and patient engagement | Contact sales | Consolidated platform for independent practices | $225/provider/month |
| Optum | Enterprise patient and member relationship layer | Contact sales | Market analytics with PRM and CRM add-ons | Custom quote |
| Actium Health | AI-driven patient activation and outreach | Contact sales | Predictive models for service line growth | Custom quote |
| Cured by Innovaccer | Unified patient data platform with CRM outreach | Contact sales | 80+ pre-built patient journeys with ML scoring | Custom quote |
| WebMD Ignite | Patient acquisition and clinical education | Contact sales | Evidence-based education in Salesforce workflows | Custom quote |
*Note: Prices may vary based on plan, billing cycle, or region. Contact vendors for healthcare-specific pricing.
1. monday CRM
Need a CRM without a long technical rollout? monday CRM gives you a flexible platform for referral pipelines, patient outreach, and care team communication. Teams can model the way referrals actually move, from the first interaction with a referring office to appointment scheduling and ongoing relationship management. The platform runs on a no-code/low-code foundation, so revenue and operations teams can adjust stages, fields, and ownership as demand shifts.

Use case: Healthcare organizations that need a flexible CRM for referral management, patient outreach, and revenue operations
Key features
- Drag-and-drop pipeline view: Manage referral pipelines with a visual layout and customizable stages. Teams use it to move referrals through clearly defined steps, while managers catch stalls early and reassign follow-up work quickly.
- Expanded item view: Keep all relevant account and contact details in one expanded item view, including connected deals and a full interaction timeline of emails, meetings, and notes. Patient coordinators see the complete history before outreach, and physician liaison teams can instantly tell what changed since the last touchpoint.
- AI voice agents: Deploy HIPAA-compliant AI voice agents that handle appointment scheduling, answer patient questions, and qualify inbound inquiries 24/7. Contact center teams reduce hold times and manual call volume while maintaining personalized patient interactions at scale.
Pricing
- Starter: $12/seat/month (billed annually)
- Standard: $17/seat/month (billed annually)
- Pro: $28/seat/month (billed annually)
- Enterprise (Ultimate): Contact sales — includes HIPAA compliance, advanced permissions, and enterprise-scale automations
- Annual billing discount: Save 18% compared to monthly billing
- Plans start from 3 seats; teams of more than 40 can request a custom quote
- Note: HIPAA compliance and Business Associate Agreement (BAA) execution are available on Enterprise (Ultimate) plans only
Why it stands out
- Fast change without heavy technical work: Revenue teams can modify boards, pipelines, dashboards, and automations to reflect their referral process without needing a large technical implementation.
- One place for the whole revenue journey: monday CRM supports lead management, deal management, account management, and post-sales workflows such as onboarding progress, renewals, and collection tracking. That matters when a “closed” referral still requires ongoing follow-through.
- HIPAA-ready AI support: monday AI is HIPAA compliant, allowing teams to use AI features inside monday CRM, including email drafting and timeline summaries, while staying aligned with healthcare compliance requirements.
2. Salesforce Health Cloud
At the enterprise end of the market, Salesforce Health Cloud brings clinical data, social determinants of health, care team details, and interaction history into one patient view. Designed for healthcare providers, payers, and public health agencies, it combines a FHIR-aligned data model with prebuilt AI agents. The result is a strong option for large organizations that need EHR interoperability at scale.

Use case: Enterprise healthcare organizations that want a unified engagement and data layer that operates alongside the EHR, linking clinical and non-clinical information to support coordinated patient and member interactions
Key features
- Patient 360 view: Unified patient profiles combine clinical records, social determinants of health, care plans, and interaction history, giving teams richer context before each touchpoint.
- FHIR-aligned interoperability: Native FHIR APIs and MuleSoft accelerators connect Health Cloud to Epic, Cerner, and other major EHRs, reducing the amount of custom integration work required.
- Agentforce for Healthcare: Prebuilt AI agents handle appointment scheduling and surface eligibility summaries, cutting down on manual lookups for contact center teams.
Pricing
- Enterprise: $350/user/month
- Unlimited: $525/user/month
- Agentforce 1 for Service: $750/user/month
- Agentforce 1 for Sales: $750/user/month
- Additional costs to factor in: Premier Success Plans are priced at 30% of net license fees and are bundled with Unlimited and Agentforce 1 editions. Add-ons like Data Cloud, MuleSoft, and Utilization Management are priced separately.
Considerations
- Mid-sized health systems often face implementation timelines of 6–12 months, and in most cases they also need dedicated Salesforce admins or certified implementation partners. In practice, that pushes the real adoption cost well beyond license pricing.
- Several important capabilities, including Utilization Management and some assessment tools, come as paid add-ons rather than standard features, which can make total costs harder to forecast at the outset.
3. HubSpot
HubSpot approaches healthcare from the growth side, combining patient acquisition, marketing automation, and contact management in one Smart CRM platform. It remains a general-purpose CRM, but private practices, wellness clinics, and health-adjacent businesses often choose it for its intuitive interface and strong marketing tooling. HIPAA compliance is possible, though not automatic: organizations need the Enterprise tier, a signed BAA, and Sensitive Data features enabled. That setup provides a governed path to patient engagement without demanding a heavy IT lift.

Use case: Healthcare organizations more focused on patient acquisition and retention than clinical workflow management
Key features
- Email marketing automation: Launch drip campaigns, segment patient audiences, and personalize outreach at scale to keep patients engaged across the care journey.
- Contact management: Maintain every patient interaction and communication history in one organized record, eliminating scattered notes and missed follow-ups.
- Landing pages and forms: Capture patient leads and manage intake within the platform using built-in form and landing page builders.
Pricing
- Free: Basic CRM functionality at no cost
- Starter: From $20/month
- Professional (Marketing Hub): From $890/month (includes 3 seats; paid onboarding required)
- Enterprise (Marketing Hub): From $3,600/month (includes 5 seats; paid onboarding required)
- Note: HIPAA support and BAA access require the Enterprise tier and enabling Sensitive Data features — a significant cost consideration for organizations handling protected health information (PHI)
- Add-ons: Brands add-on ($1,000/month), custom objects ($500/month), and AI/automation credits ($0.010 per credit) can increase total cost
Considerations
- Out-of-the-box HIPAA compliance is not available on lower plans. To support it, organizations need Enterprise-tier access, a BAA, and the correct Sensitive Data configuration; once Sensitive Data is enabled, it cannot be disabled.
- Because HubSpot lacks native clinical or EHR workflows, practices handling referrals or clinical coordination will need custom builds or third-party integrations.
4. Zendesk
Where patient communications create the main operational load, Zendesk is often the better fit. It gives healthcare organizations one platform for managing support requests across phone, email, chat, and messaging. Providers, payers, and healthcare vendors use it to run secure, omnichannel engagement without replacing their EHR.

Use case: Healthcare contact centers and patient services teams that need to handle large volumes of inquiries across multiple channels from a single compliant inbox
Key features
- Omnichannel ticketing: Brings patient communications from phone, email, chat, and messaging into one unified inbox, reducing the risk that inquiries get missed.
- HIPAA-enabled compliance: Supports HIPAA coverage through a BAA and the Advanced Compliance add-on, with Zendesk AI also eligible for inclusion under the BAA.
- Reporting and analytics: Monitors call volume, response times, and patient satisfaction through built-in and custom dashboards, giving patient services leaders clear reporting data.
Pricing
- Suite Team: $49/agent/month (billed annually)
- Suite Growth: $79/agent/month (billed annually)
- Suite Professional: $99/agent/month (billed annually)
- Suite Enterprise: $150/agent/month (billed annually)
- Suite + Copilot bundles: $155/agent/month (Professional) and $209/agent/month (Enterprise), billed annually
- Add-ons available separately: Copilot ($50), Quality Assurance ($35), Workforce Management ($25), Advanced Data Privacy & Protection ($50), and Contact Center ($50), all billed annually per agent
- HIPAA enablement requires the Advanced Compliance add-on and is not included by default
Considerations
- Zendesk is optimized for patient support rather than revenue operations. Organizations that need referral pipeline management, deal tracking, or revenue cycle visibility will run into limits.
- To get HIPAA coverage, teams must purchase the Advanced Compliance add-on, sign a BAA, and meet specific security requirements. SMS is excluded from HIPAA-enabled Talk coverage, and many Marketplace apps are outside the scope of PHI handling.
5. Microsoft Cloud for Healthcare
For organizations already invested in Microsoft, this platform can feel like the natural extension of the existing stack. Microsoft Cloud for Healthcare combines Dynamics 365 CRM, Microsoft Teams, and Azure Health Data Services into an enterprise platform for large health systems. It serves healthcare providers, payors, and life sciences organizations that want a composable set of CRM and collaboration tools without leaving the Microsoft ecosystem. One standout feature is its FHIR-based data virtualization, which allows CRM workflows to read directly from clinical sources instead of relying on bulk data replication.

Use case: Large health systems that want CRM, care coordination, and clinical data integration inside a unified Microsoft environment
Key features
- Unified patient view: A single Dynamics 365 interface displays patient demographics, clinical timelines, care team details, and FHIR-linked data, with security-role separation between clinical and administrative views.
- FHIR-based data interoperability: The FHIRlink connector and virtual health data tables let CRM apps and automated workflows connect directly to FHIR endpoints, including Epic and Azure Health Data Services, without copying the underlying data.
- Teams and EHR integration: Care teams can manage virtual visits, agent workflows, and contact center interactions through Microsoft Teams, with connectors to major EHR systems providing clinical context.
Pricing
- Dynamics 365 Customer Service Professional: $50/user/month
- Dynamics 365 Customer Service Enterprise: $105/user/month
- Dynamics 365 Customer Service Premium: $195/user/month
- Dynamics 365 Customer Insights: From $1,700/tenant/month
- Microsoft Cloud for Healthcare add-on: Custom pricing — requires existing Dynamics 365, Microsoft 365, Power Platform, and Azure licensing; contact Microsoft sales for a full quote
- Additional costs: Voice and SMS capabilities are billed separately through Azure Communication Services; Copilot capacity, Power BI, and other services may require additional licenses or Azure consumption
Considerations
- New customers can no longer deploy the packaged Patient Outreach and Patient Service Center apps through the Power Platform admin center; new implementations now require custom solutions built with Dynamics 365, Microsoft Fabric, and connectors, which adds substantial configuration time.
- Predicting total cost of ownership is difficult up front because healthcare CRM use cases usually require multiple licenses spanning Dynamics 365, Microsoft 365, Power Platform, and Azure. That makes it a weak match for organizations seeking fast deployment or predictable pricing.
6. Epic
Some health systems want CRM functionality inside the EHR they already trust, and that is exactly where Epic positions Cheers. Epic’s reputation was built on clinical operations, and Cheers extends that footprint into patient engagement and acquisition.

Use case: Health systems already running Epic that need a purpose-built CRM layer that links patient outreach, scheduling, and care gap management inside one clinically integrated ecosystem
Key features
- Closed-loop campaign tracking: Cheers measures engagement metrics such as opens and clicks, then ties outcomes like appointments scheduled, preventive screenings completed, and revenue generated back to specific campaigns.
- Capacity-aware outreach: Outreach populations shift automatically based on near-term appointment availability, keeping campaigns aligned with real scheduling capacity instead of creating unmanageable demand.
- Caller 360 and provider matching: The Cheers Call Management module shows a caller’s full interaction history, from scheduling to billing, and uses Provider Finder to route patients to accepting clinicians in real time.
Pricing
- Bundled with Epic EHR licensing: No standalone CRM pricing is available; organizations engage Epic directly for a custom quote.
- Additional costs may apply for third-party contact center integrations (e.g., NICE CXone, Talkdesk) and SMS carrier fees for patient outreach programs.
Considerations
- Cheers only exists within the Epic world. It is not sold as a standalone CRM and is designed exclusively for organizations using the Epic EHR. Epic does support interoperability for data exchange through FHIR APIs, but Cheers itself cannot be purchased or implemented independently.
- Epic implementations at the enterprise level involve substantial total cost, making it a major commitment, especially for organizations evaluating CRM as a standalone need.
7. Zoho for healthcare
Not every healthcare organization needs an enterprise budget to get CRM functionality. Zoho provides a broad, configurable option for teams that need patient contact management, appointment coordination, and outreach automation at a lower cost. It appeals mainly to smaller practices and health-adjacent businesses that want flexibility across the patient lifecycle.

Use case: Smaller healthcare organizations and health-adjacent businesses that need an adaptable CRM for patient relationships, automated follow-ups, and appointment coordination across channels
Key features
- Omnichannel patient communication: Connect with patients through WhatsApp, SMS, email, and chatbots from one platform, using templated messaging and automated reminders to reduce no-shows.
- Appointment scheduling and telehealth support: Sync virtual and in-person appointments with Zoho Calendar or Google Calendar, with automated notifications and no-show tracking included.
- EHR/HIMS integration: Link Zoho CRM to existing clinical systems so patient engagement data and operational workflows remain coordinated without replacing the primary records platform.
Pricing
- Standard: $14/user/month (billed annually) or $20/user/month (billed monthly)
- Professional: $23/user/month (billed annually) or $35/user/month (billed monthly)
- Enterprise: $40/user/month (billed annually) or $50/user/month (billed monthly)
- Ultimate: $52/user/month (billed annually) or $65/user/month (billed monthly)
- HIPAA compliance features are available on Standard plans and above — not included in the free tier
- Annual billing saves up to 34% compared to monthly pricing
- Premium support plans are available at an additional cost (20–25% of subscription fee)
Considerations
- Reaching HIPAA compliance requires careful configuration, a signed BAA, and a clear understanding of which features are within scope. Teams handling PHI need to budget time for proper setup before launch.
- Zoho does not come with prebuilt healthcare workflows. Organizations must configure their own processes, which adds setup effort and may require help from Zoho’s solutions team rather than a purely self-service rollout.
8. LeadSquared
LeadSquared sits in a middle ground many healthcare organizations find appealing: it is more healthcare-focused than a general CRM, but typically faster to deploy than heavyweight enterprise platforms. Its AI-powered sales and marketing platform supports patient acquisition, intake, and engagement within a HIPAA-compliant framework. Hospitals, multi-location clinics, and healthcare networks use it to manage the full patient journey from initial inquiry to ongoing care.

Use case: Hospitals and healthcare networks use LeadSquared to capture, route, and convert patient inquiries more quickly by combining HIPAA-compliant communications, referral management, and appointment automation in one platform
Key features
- Multichannel patient outreach: Engage patients across SMS, email, WhatsApp, chatbots, and phone within a HIPAA-compliant framework, keeping every channel under management.
- Appointment management and no-show reduction: Automated booking, calendar sync, and reminder workflows help keep schedules full and patients informed before arrival.
- EHR and HMS integrations: Connectors for Epic, Athenahealth, DrChrono, and eClinicalWorks help synchronize patient and appointment data across systems, reducing manual work.
Pricing
- Sales CRM (billed annually):
- Pro: $60/user per month
- Super: $100/user per month
- Marketing Automation (billed annually):
- Pro: $2,000 per account per year
- Super: $3,500 per account per year
- Special pricing is available for select startups; volume and enterprise discounts are handled through the sales team.
- Several capabilities — including portals, the HL7 EHR connector, AI email parser, and analytics modules — are available as paid add-ons, which can increase total cost depending on integration depth.
Considerations
- The HL7 EHR connector is only available to US-based healthcare customers, requires setup through the account team, and is sold as a paid add-on. Organizations with complex or multi-system EHR environments should account for extra time and cost.
- Some G2 reviewers report occasional UI slowness and constraints in advanced reporting, which may be a drawback for teams that depend heavily on real-time executive analytics.
9. Creatio
Some organizations do not need a prepackaged healthcare CRM as much as they need a platform they can shape themselves. Creatio is built for exactly that. It is a no-code CRM and process automation platform aimed at mid-market and enterprise healthcare teams, including hospital systems, payers, telehealth providers, and life sciences organizations that have outgrown rigid systems. With agentic AI embedded directly into its workflow engine, operations teams can design and adapt patient journeys without writing code.

Use case: Healthcare organizations with complex, process-heavy requirements seeking a configurable CRM for patient engagement, referral workflows, and care coordination across multiple systems
Key features
- No-code workflow builder: Create and adjust patient journey workflows, referral management processes, and care coordination automations with a visual designer and no developer involvement.
- EHR and EMR integration: Connect to major systems such as Epic, Oracle Health/Cerner, Athenahealth, and Meditech through Marketplace connectors, helping keep patient data synchronized.
- HIPAA-aligned security: SOC 2 Type II certified with ISO 27001 alignment, tenant-isolated databases, and built-in HIPAA guardrails to support compliant PHI handling.
Pricing
- Platform: Starting from $25/user/month
- CRM products (Marketing, Sales, or Service): $15/user/month each, added as needed
- Bundled starting price: From $40/user/month (platform + one CRM product)
- Detailed pricing is quote-based; marketplace apps and connectors are billed separately on annual subscriptions and do not include the core platform license.
Considerations
- That flexibility comes with real setup work. Most organizations need dedicated operations staff or an implementation partner to design and build workflows before launch, which lengthens time to value compared with pre-configured healthcare CRMs.
- A number of specialized capabilities, including contact center integrations, chatbots, and some EHR connectors, depend on Marketplace apps with separate subscription fees. Total ownership cost can rise quickly depending on the integrations required.
10. NexHealth
At the practice level, NexHealth focuses less on pipeline management and more on making patient engagement repeatable. It is designed specifically for healthcare providers and ties scheduling, messaging, and intake forms directly to the EHR, helping front-desk teams spend less time tracking people down.

Use case: Dental, medical, and specialty practices that want to automate patient-facing workflows, from online booking to post-visit review requests, while remaining inside their existing EHR ecosystem
Key features
- Real-time online scheduling: Patients can book appointments 24/7 from your website, SMS, email, or Google, with those appointments written directly to the schedule to avoid double-booking.
- Two-way HIPAA-compliant messaging: A centralized inbox manages text and email communication from the office number, with smart reminders that skip patients who already confirmed or rescheduled.
- One-Click Recalls: Automated recall messages include pre-filled patient details and live available time slots, triggered by due dates and procedure codes pulled directly from the EHR.
Pricing
- Custom pricing: Quote-based, configured per practice size and feature selection.
- Annual billing discount: Pay for 12 months and get 1 month free at your current monthly rate.
- Usage inclusions to note: 5,000 campaign SMS texts per location per month included; overages billed at $0.012 per SMS. Insurance verification included up to 800 per month; $0.20 per verification after that.
- Payment processing fees: 2.9% + $0.30 for online and text-to-pay; 2.6% + $0.07 for terminals.
Considerations
- NexHealth is centered on patient engagement and front-desk workflows. Organizations that need referral pipeline tracking, revenue forecasting, or cross-department operational workflows will need something more.
- Some automations depend on the connected EHR or practice management system, and certain features, including rescheduled appointment triggers, have limitations with specific integrations.
11. Tebra
For independent practices trying to consolidate vendors, Tebra deserves attention. The platform combines EHR, billing, practice management, and patient engagement in one system tailored to smaller medical groups. Formed through the 2021 merger of Kareo and PatientPop, if simplifying the stack matters more than building a sophisticated sales pipeline, it is a practical option.

Use case: Small to midsized independent practices that want one platform for clinical, financial, and patient communication workflows rather than a patchwork of separate vendors
Key features
- Patient acquisition and visibility: Web profiles sync across Google and 80+ directories, helping route new patients directly into real-time online scheduling.
- HIPAA-compliant patient engagement: Two-way SMS, broadcast messaging, digital intake with e-signatures, and automated reminders.
- AI-powered reputation management: Automated review requests, AI Review Replies, and AI Review Insights dashboards surface sentiment trends across patient feedback.
Pricing
- Physician Standard (Essentials): $599/provider/month
- Physician Standard (Automation): $799/provider/month
- Physician Low-Volume (Essentials): Starting at $349/provider/month
- Non-physician Standard (Essentials): $399/provider/month
- Therapist Standard (Essentials): $225/provider/month
- Patient Experience + Marketing (single solution): Starting at $49/provider/month (non-physician) or $99/provider/month (physician)
- EHR Starter (single solution): Starting at $99/provider/month (non-physician) or $199/provider/month (physician)
- Non-clinical staff seats are included at no extra cost across plans
- Add-on fees apply for EPCS setup, PDMP access, telecom messaging compliance, credit card processing, and optional AI note generation
Considerations
- Tebra does not include a dedicated CRM module. Its patient engagement tools live inside the Patient Experience and Practice Marketing products, so practices needing traditional pipeline management or multi-location revenue operations will find the offering limited.
- Care Connect and growth capabilities are primarily U.S.-focused, and overall costs can rise noticeably once add-ons and pass-through fees are added to the base subscription.
12. Optum
Optum is less a standalone CRM product than an enterprise operating layer for patient and member relationships. Built on UnitedHealth Group’s large-scale data infrastructure, it embeds CRM capabilities into workflows involving scheduling, eligibility, communications, and analytics.

Use case: Health plans and large integrated delivery networks that manage patient and member relationships across the care journey, from acquisition and scheduling through retention and financial communication
Key features
- Patient access and engagement: Multichannel scheduling, digital intake, automated reminders, and eligibility verification. Intake and eligibility functions are integrated at the EHR field level, helping reduce manual entry and administrative errors.
- Optum Market Advantage (OMA) with PRM and CRM add-ons: Brings together local market analytics with physician relationship management and patient outreach, giving growth teams modeled loyalty data, leakage analysis, and campaign ROI tracking.
- Member engagement for payers: Multi-channel outreach, live advocate support, and activation workflows designed specifically for health plan member engagement and retention.
Pricing
- Enterprise only: Pricing is quote-based and negotiated based on scope, modules selected, and organizational size — no public tiers are available.
- CRM and PRM capabilities within OMA are available as add-ons for an additional fee.
- Implementation services, contact center operations, and communications modules may be scoped separately.
Considerations
- Optum’s solutions are aimed mainly at health plans and large health systems. Smaller practices or teams searching for a general-purpose CRM will usually find it outside their scope.
- Overall cost depends heavily on module selection, the degree of EHR and data integration required, and whether contact center services are part of the deal, so evaluating value typically requires a full scoping engagement.
13. Actium Health
Actium Health takes a narrower, activation-focused approach. Its core value lies in using AI to determine which patients are most likely to need care next, then reaching them automatically across voice, SMS, chat, and email. The platform is designed for large health systems and integrated delivery networks.

Use case: Health systems looking to proactively activate patients and grow service line revenue through AI-driven, multi-channel outreach
Key features
- AI patient prioritization: Predictive models review EHR and claims data to determine which patients are most likely to need certain services, helping teams focus outreach where it matters most.
- Automated multi-channel outreach: Manages personalized engagement across voice, SMS, chat, and email.
- EHR-integrated scheduling: Connects directly to existing EHR systems to close care gaps and convert outreach into booked appointments.
Pricing
- Custom pricing: Quote-only, based on call volume, number of locations, selected features, and EHR integration requirements.
Considerations
- Actium Health is designed for outbound patient activation and inbound communication automation rather than serving as a full CRM system of record. Health systems will still need a separate platform for broader relationship management, referral tracking, and collaboration.
- Documentation around CRM and provider relationship management features appears mostly in legacy help center materials, so organizations assessing it as a standalone CRM should verify current scope and roadmap directly with the vendor.
14. Cured by Innovaccer
Cured by Innovaccer is built around a simple idea: unify patient data first, then make outreach smarter. It combines a healthcare consumer data platform with CRM-driven engagement so large provider organizations can run targeted campaigns without building the underlying data infrastructure themselves. The platform is geared toward integrated delivery networks and health systems that want to connect clinical, claims, and behavioral data with marketing automation inside one vertically integrated stack.

Use case: Large U.S. health systems that want to activate unified patient data for omnichannel outreach, care gap campaigns, and access center workflows
Key features
- Healthcare consumer data platform: Unifies clinical, demographic, behavioral, and third-party data, including Experian attributes, into a Patient 360, with 80+ pre-built integrations across major EHRs such as Epic, Oracle Cerner, and MEDITECH.
- Pre-built patient journeys: Provides 80+ ready-made healthcare journeys called “Curations,” along with ML propensity scoring to target high-likelihood patient segments across email, SMS, and portal channels.
- Access center integration: Links CRM outreach directly to AI-enabled contact center workflows, including call summaries, next-best-action prompts, and automated task routing, to reduce leakage between patient interest and booked appointments.
Pricing:
- Custom pricing: Keep in mind that certain certified capabilities available on the broader Innovaccer platform, such as eCQM reporting, may be add-ons that incur costs beyond the Cured offering.
Considerations
- Cured by Innovaccer delivers its greatest value when paired with the broader Innovaccer data infrastructure. Without that foundation, some capabilities will be limited or unavailable.
- Much of the published performance evidence comes from vendor-reported case results. Independent third-party validation is limited in public sources.
15. WebMD Ignite
WebMD Ignite brings together patient engagement, clinical education, and healthcare marketing, leaning heavily on the reach of the broader WebMD ecosystem. For health systems and payers focused on consumer-facing growth, that reach matters. The platform is especially notable for pairing healthcare-specific data with acquisition and engagement tools.

Use case: Health systems and payers that want to run targeted patient acquisition campaigns, deliver clinically reviewed education, and measure ROI across service lines
Key features
- Ignite Growth Platform: Combines market planning insights, audience targeting, campaign performance tracking, and referral growth analytics to identify service-line opportunities and reduce patient leakage.
- IntegratED for CRM: Places evidence-based patient education directly into Salesforce workflows, with historical education logs and multi-channel delivery through email or SMS.
- Data-as-a-Service (DaaS): Enriches existing CRMs and marketing automation tools with predictive clinical models and consumer patient profiles, allowing organizations to activate data without replacing current systems.
Pricing
- Custom pricing: Quote-only; no public pricing is available. Organizations are directed to schedule a consultation or demo for a tailored quote.
Considerations
- WebMD Ignite’s CRM integration is geared primarily toward Salesforce, so organizations using other CRM platforms may find out-of-the-box connectivity limited.
- The platform is centered on patient acquisition and education rather than operational CRM workflows like referral management, revenue cycle visibility, or cross-team pipeline tracking. Health systems that need those capabilities will need additional tools.
6 reasons healthcare organizations use a CRM
In healthcare, relationships drive everything. Yet many back offices still run on spreadsheets, disconnected tools, and half-complete handoffs. A CRM brings order to the operational mess, handling the follow-ups, referrals, and outreach that determine whether patients show up, return, and stay connected.
- Stronger patient engagement and retention: A CRM automates follow-ups and recall campaigns, turning static records into active relationships that keep patients engaged and coming back.
- Coordinated care across departments: Billing teams, care navigators, and front-office staff work from the same interaction history, eliminating the miscommunication that throws off the patient experience.
- Visibility into referrals and the revenue cycle: A live view of the referral pipeline makes it easier to identify high-value partners and spot where patients are falling out of the process.
- Reduced administrative burden for staff: Automating repetitive tasks such as intake forms, reminders, and follow-ups reduces manual data entry and frees staff to spend more time on patients.
- Personalized outreach at scale: Segment patients based on condition, care gaps, or interaction history to deliver relevant communication instead of generic mass messaging.
- Cross-team collaboration beyond the front desk: A CRM connects marketing, physician relations, and revenue teams around one shared system, reducing silos and making strategic decisions easier.
7 features to look for in healthcare CRM software
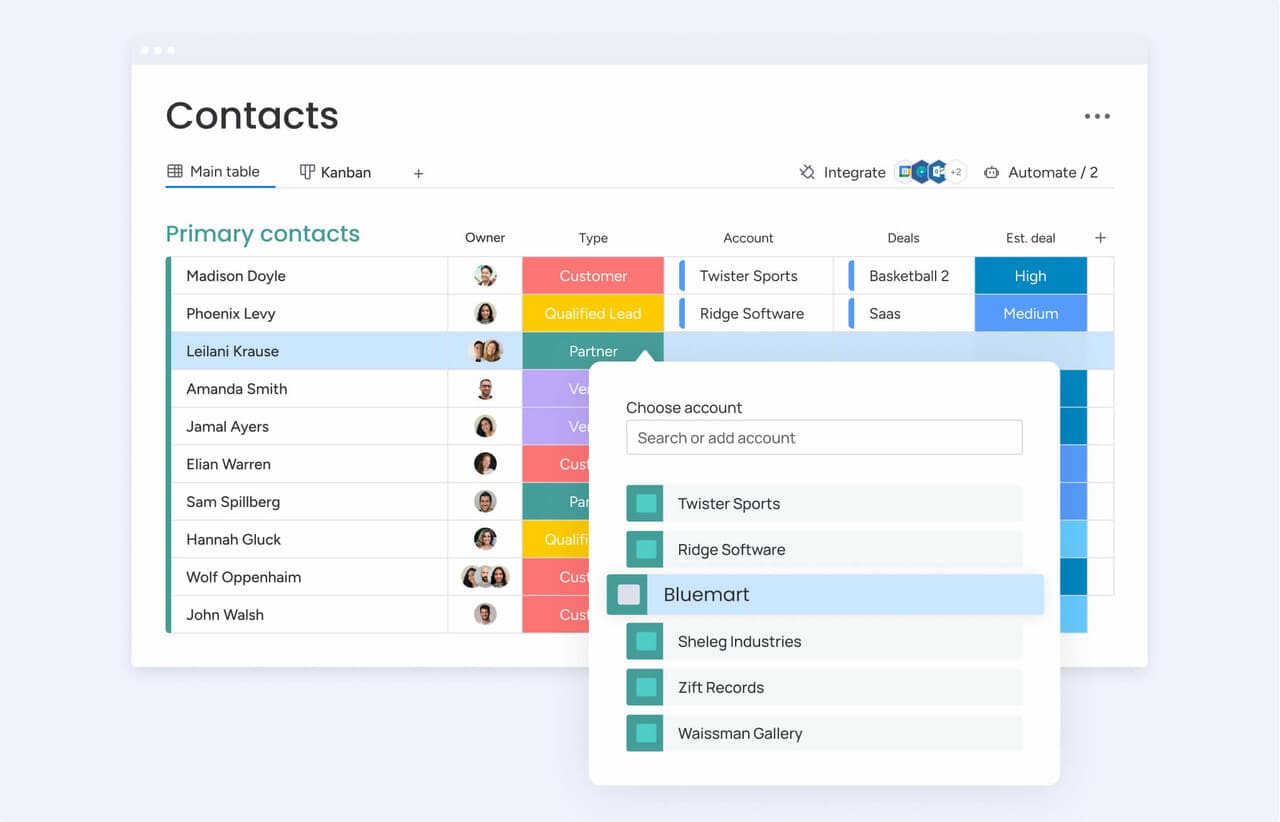
Plenty of tools market themselves as healthcare CRMs while functioning more like generic sales software with minimal adaptation. The difference between a platform that actually helps and one that creates more drag is enormous. These are the features that separate a real operational partner from a glorified spreadsheet.
- Centralized patient and contact records: Emails, calls, notes, and referral history all belong in one CRM database, on one screen. That way, no one starts a call by guessing what happened last.
- Referral and pipeline management: A solid CRM provides a visual pipeline that tracks each referral from source to scheduled appointment. At any moment, you should be able to see exactly where every opportunity stands.
- Workflow automation and AI: Look for a platform that automates tasks such as appointment reminders and status changes without requiring developer support. And AI should do real work, not just sound impressive. It should help draft emails, extract details from documents, and give time back to the team.
- Multi-channel patient communication: A strong CRM combines email, SMS, and phone logs in one interface. Care coordinators can then see who opened an outreach message, who responded, and who still needs a call without hopping between tools.
- Custom dashboards and reporting: Referral volume and pipeline health need to be visible in real time. Effective platforms let teams build dashboards themselves with zero code, so answers do not depend on analyst queues.
- Critical tech stack integrations: A CRM that cannot connect with your EHR or billing platform does more harm than good. Deep integration with your existing systems is not optional. If the software creates another silo, it is a step backward.
- HIPAA-grade security: There is no gray area here. If a platform is not HIPAA compliant, it is out. Full stop. You need a signed Business Associate Agreement (BAA), end-to-end encryption, and granular permissions that control exactly who can access patient data.
This is not an aspirational checklist. It is the minimum standard for a healthcare CRM that pulls its weight. Revenue teams find success using monday CRM to bring these functions together, turning the platform into something the team depends on rather than works around.
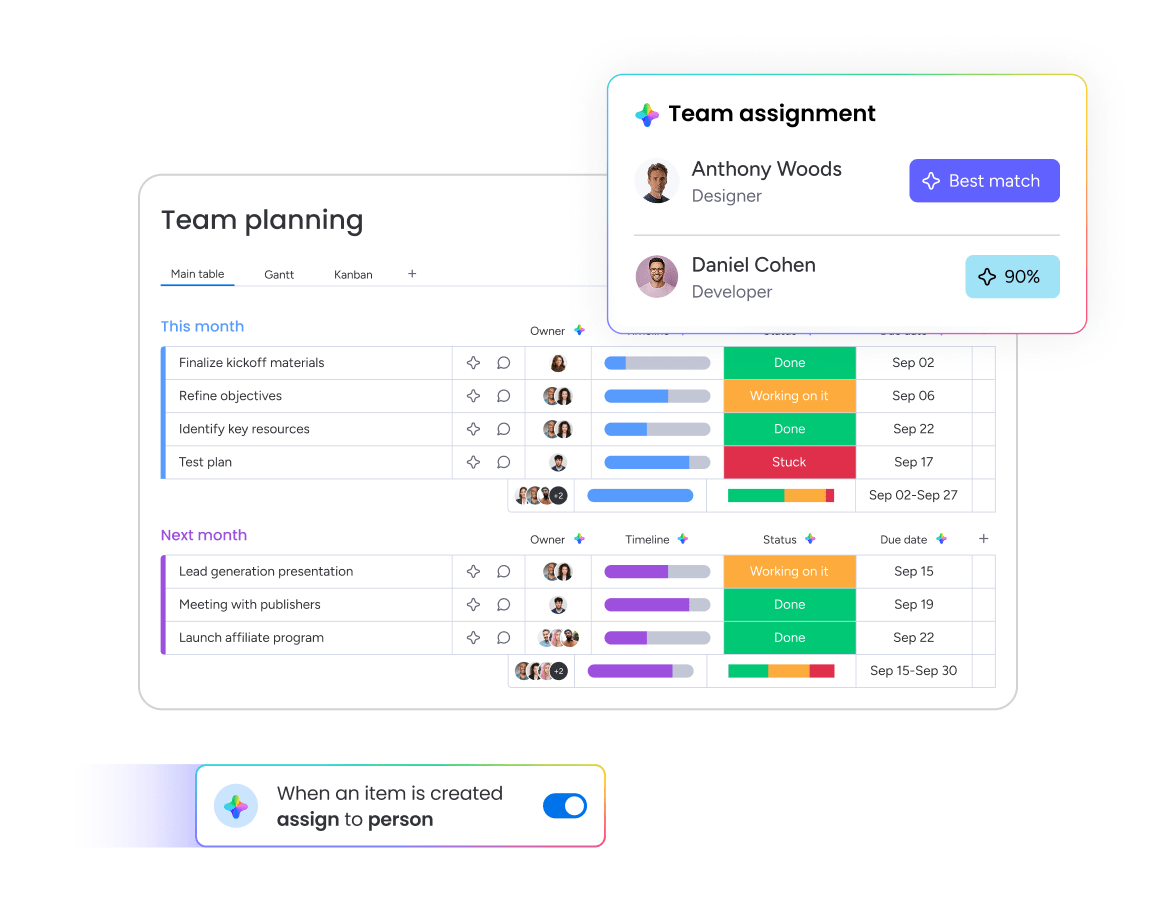
HIPAA compliance and data security in healthcare CRM
HIPAA compliance is a starting point — not a feature request for later. The moment a CRM stores patient details or communication history, it is handling protected health information (PHI), and the compliance stakes rise immediately.
Mistakes here are more than inconvenient; they create serious legal exposure. Before you evaluate dashboards, workflows, or automations, ask vendors a basic question: Do you offer a Business Associate Agreement (BAA)? That agreement is the legal prerequisite for storing PHI in a CRM compliantly.
Revenue teams find success using monday CRM to centralize patient data because it supports HIPAA compliance and BAA execution on qualifying plans, while providing the core technical safeguards organizations need.
- Encryption: Protects PHI with AES-256 encryption at rest and TLS 1.3 in transit.
- Audit logs: Records who accessed patient data and when, creating a detailed activity trail.
- Role-based access: Limits visibility so front desk teams, billing staff, and clinicians only see the information relevant to their role.
Keep in mind that HIPAA establishes the federal baseline, not the entire compliance picture. Many states impose stricter requirements. Getting this right from day one protects the organization and reinforces patient trust in a way marketing never can.
Try monday CRMHow a healthcare CRM connects with your EHR
Your EHR holds patient data. Your CRM holds relationship data. When they don’t talk to each other, your staff wastes time on manual entry — and that creates errors.
The fix is integration. Most modern CRMs connect to EHRs through standard APIs or middleware platforms, so patient information flows automatically between systems. That means your team sees the full picture without jumping between screens.
Done well, integration removes work instead of creating it. Organizations find success using monday CRM because its open API and integrations connect with major EHR systems, helping teams spend less time wrangling data and more time serving patients.
5 steps to choose the right healthcare CRM

Selecting a healthcare CRM is not just a software decision. It shapes how your team operates, how patients experience your organization, and how the practice grows over time. Choose poorly, and the result is frustrated staff, wasted budget, and preventable gaps in care.
These 5 steps make the decision more grounded and less risky.
- Map your real-world workflows: Walk through the patient journey as it actually happens and listen to the people doing the work. Front-desk coordinators know why reminders fail, and revenue analysts know where referral tracking breaks down.
- Define your non-negotiables: Write down your deal-breakers first—HIPAA BAA requirements, must-have EHR integrations, and billing platform connections. Use this as a filter to narrow the field quickly.
- Focus on roles, not just features: Pick 2–3 key roles and define their top 3 workflows. Features only matter if they solve the right problem for the people who will live in the system every day.
- Prioritize adoption and ease of use: Ask practical questions: How quickly can we launch? Can business teams build workflows without IT? A no-code platform like monday CRM lets teams configure what they need in days rather than months.
- Pilot your top choice: Start with a structured pilot involving one team and a clearly defined goal. Measure outcomes such as reduced no-show rates or faster referral conversion before expanding across the organization.
Building a patient-first revenue engine
Healthcare operations do not slow down, and neither can the systems supporting them. A dedicated CRM helps close the gap between clinical care and the business side of the practice so referrals, follow-ups, and outreach do not get lost. For revenue and operations teams, that visibility is what makes predictable growth possible.
The best platform fits your workflows instead of forcing your teams into someone else’s model. Centralized communication, automated manual work, and EHR integration all reduce friction. Begin with your biggest operational bottlenecks and your non-negotiables. Once those are clear, evaluating platforms and running a focused pilot becomes a far more confident process.
Try monday CRMFAQs
How does a CRM differ from an EHR?
An EHR manages clinical records and medical history during the appointment, while a CRM handles the relationship and administrative work surrounding the appointment. Together, they provide a more complete view of the patient journey.
Is a healthcare CRM HIPAA compliant?
It can be. A healthcare CRM may be HIPAA compliant if the vendor offers a Business Associate Agreement (BAA) and includes safeguards such as encryption and role-based access controls. Always confirm those capabilities before implementation.
Why do hospitals need a CRM?
Hospitals use CRMs to coordinate care across departments, manage large referral pipelines, and personalize outreach at scale. The platform centralizes communication so revenue and operations teams can work from a single source of truth.
Can a CRM integrate with Epic or other EHRs?
Yes. Modern CRMs can connect with Epic and other EHRs through direct APIs, middleware, or FHIR-based integrations. That keeps relationship data and clinical records in sync without relying on manual entry.
What are the main benefits of using a CRM in healthcare?
The biggest benefits include stronger patient retention, lower administrative burden, and clearer visibility into the revenue cycle. By automating repetitive work, a CRM gives staff more time for high-value patient interactions.

